Joint Commission Equipment Checklist
Purchasing medical equipment is not just a clinical or operational decision. It is an accreditation decision.
For purchasing teams, IT directors, OB leaders, and facilities staff, equipment choices directly impact preventive maintenance programs, documentation requirements, infection prevention policies, and survey readiness. Selecting the wrong cart, power strip, or surface material can create additional policy complexity or result in survey findings that require corrective action.
This guide outlines key Joint Commission considerations and practical equipment checkpoints to help healthcare buyers make informed decisions that support accreditation readiness.
Table of Contents
- Understanding The Joint Commission Requirements
- General Equipment Management and Maintenance Documentation
- Medical Equipment Requirements: Emergency Carts
- Medical Equipment Requirements: Postpartum Hemorrhage Carts
- Medical Equipment Requirements: Labor and Delivery Carts and Furniture
- Medical Equipment Requirements: Computers on Wheels
- Medical Equipment Requirements: Medication Delivery
- Medical Equipment Requirements: Electrical Safety and UL Standards
- What To Do After Receiving New Equipment
- Staying Survey Ready
- Frequently Asked Questions
1) Understanding The Joint Commission Requirements
1.1) What is The Joint Commission?
The Joint Commission (TJC) is a CMS-recognized accrediting organization that evaluates healthcare facilities for compliance with patient safety, infection prevention, and Environment of Care standards.
Hospitals may also choose other CMS-approved accreditation agencies such as DNV or HFAP. CMS maintains a current list of accrediting organizations for prospective clients. Regardless of the accrediting body, facilities must meet CMS Conditions of Participation to maintain reimbursement eligibility.

Accreditation affects:
- Patient safety protocols
- Infection prevention programs
- Equipment maintenance policies
- Documentation standards
For healthcare buyers, this means purchasing decisions influence more than clinical workflow. They shape compliance requirements.
1.2) Environment of Care Considerations
Many Joint Commission expectations for equipment live under the Environment of Care framework. In practical terms, surveyors want to see that your organization can identify medical equipment, determine which devices are higher risk, and demonstrate that inspection, testing, and maintenance occur on schedule and are documented. The equipment itself matters, but so does your organization’s ability to manage it reliably.
1.3) Broader Equipment Compliance Considerations
In addition to TJC standards, facilities should align equipment purchases with:
- TIP Test expectations for ligature risk in behavioral health environments
- ISO 9001:2015 quality and risk management principles, particularly for DNV-accredited facilities
- UL and IEC electrical safety certifications, including UL 60601-1 and UL 1363A for medical electrical equipment
IT and clinical engineering teams should confirm certifications before purchase, as retroactive compliance adjustments can increase cost and documentation burden.
1.4) Lessons Learned From Real Survey Findings
As a healthcare equipment provider, we track common equipment-related survey findings reported by facilities following Joint Commission walkthroughs.
Frequently cited concerns include:
- Porous wood carts and furniture in clinical areas
- Use of hook and loop fasteners in patient care environments
- Damaged surfaces that compromise cleanability
- Equipment that lacks clear identification or maintenance traceability
These are not abstract standards. They are practical findings that often require replacement, remediation, or policy updates.
1.5) What This Blog Covers
Below, we outline several equipment categories that require special consideration from an accreditation standpoint, with a focus on how purchasing decisions influence compliance.
While we work closely with healthcare facilities on equipment compliance, we are not an accrediting body. Always refer to official Joint Commission guidance and your accrediting organization for definitive requirements.

2) General Equipment Management and Maintenance Documentation
Before surveyors examine equipment, they review documentation.
2.1) Inventory and Asset Tracking
Checklist:
- Maintain a complete, current inventory of all medical equipment, including identification of high-risk and life-support devices
- Ensure each piece of equipment can be clearly identified and traced to maintenance and inspection records. Many facilities use asset tags or barcode systems to support this requirement
From a purchasing perspective, consider how easily new equipment can be integrated into your CMMS and tracking systems before placing orders.

2.2) Preventive Maintenance and Inspection Records
Checklist:
- Preventive maintenance schedules align with manufacturer recommendations
- Alternative Equipment Maintenance (AEM) documentation is available if used
- Calibration and safety testing logs are accessible for review
Equipment without clear manufacturer maintenance instructions can increase policy development work for clinical engineering and facilities teams. Buyers can reduce downstream work by confirming that maintenance guidance and documentation are available at time of purchase.
3) TJC Medical Equipment Requirements: Emergency Carts
Emergency carts are frequently reviewed during surveys because they combine medication access, equipment readiness, and operational reliability.
3.1) Cart Construction and Cleanability
Checklist:
- Non-porous cart surfaces that are easy to disinfect
- Readily accessible for immediate use
Selecting carts constructed with healthcare-grade materials helps ensure long-term durability, supports infection prevention protocols, and reduces the likelihood of surface-related survey findings.

3.2) Equipment and Supply Readiness
Joint Commission guidance states that locking devices that create delays or barriers to immediate access may be interpreted as not readily accessible for use. Breakaway tags with numeric identification numbers are acceptable if there is a defined monitoring process in place.
Checklist:
- Tamper seals intact and replaced after use
- High-risk equipment such as portable suction units and AEDs inspected per manufacturer instructions
Purchasing teams should confirm that carts support breakaway tag systems rather than complex locking mechanisms that may raise accessibility concerns. When carts require special keys or slow access, facilities often have to create extra procedures to justify readiness.

3.3) What Surveyors Often Do in Practice
During tracers, surveyors may ask staff to identify the cart, confirm it is in the expected location, and explain how integrity checks are performed. They may also look at surface condition, labels, and whether the cart can be cleaned effectively using approved disinfectants. A cart that is hard to clean or hard to access can create compliance concerns even if it is stocked correctly.
4) TJC Medical Equipment Requirements: Postpartum Hemorrhage Carts
Postpartum hemorrhage carts share similarities with emergency carts but carry additional scrutiny under Joint Commission’s Provision of Care, Treatment, and Services standards for maternal safety. Read our blog about it here.
4.1) Cart Construction and Cleanability
Checklist:
- Non-porous, seamless cart surfaces
- Drawers and handles easy to disinfect
- Immediate accessibility consistent with emergency cart guidance
4.2) Standardization and Accessibility
Checklist:
- Standardized cart layout across units
- Approved procedures documented
- Locked and controlled access to medications
- Immediate availability during obstetric emergencies
Standardization reduces confusion during clinical events and supports policy compliance. From a buyer standpoint, purchasing the same cart model across units can reduce variation, simplify training, and make stocking and documentation more consistent.
5) TJC Medical Equipment Requirements: Labor and Delivery Carts and Furniture
Historically, many bassinets, fetal monitor carts, and L&D furniture components were constructed using wood.
Joint Commission correspondence has clarified that if surfaces are porous or not cleanable, they do not provide a surface that can be appropriately disinfected, and therefore may not meet accreditation expectations.
As a result:
- Labor and delivery carts should be non-porous
- Wood components in patient care areas may require replacement
- Surfaces must withstand hospital-grade disinfectants
Purchasing non-porous alternatives reduces the risk of future replacement requests and can help infection prevention teams standardize cleaning procedures.

6) TJC Medical Equipment Requirements: Computer on Wheels
Computers on Wheels (COWs), or mobile workstations, are frequently evaluated during accreditation surveys due to their impact on infection prevention, electrical safety, and Life Safety requirements.
One key consideration is storage. COWs should not be parked in corridors when not in use, especially for charging, as this can obstruct egress and conflict with Life Safety expectations. Facilities should plan for designated storage and charging areas.
6.1) EMR Cart Construction and Cleanability
Checklist:
- Non-porous, cleanable cart surfaces
- Durable surfaces that withstand hospital-grade disinfectants
- Cleanable keyboards, mice, and touchpoints
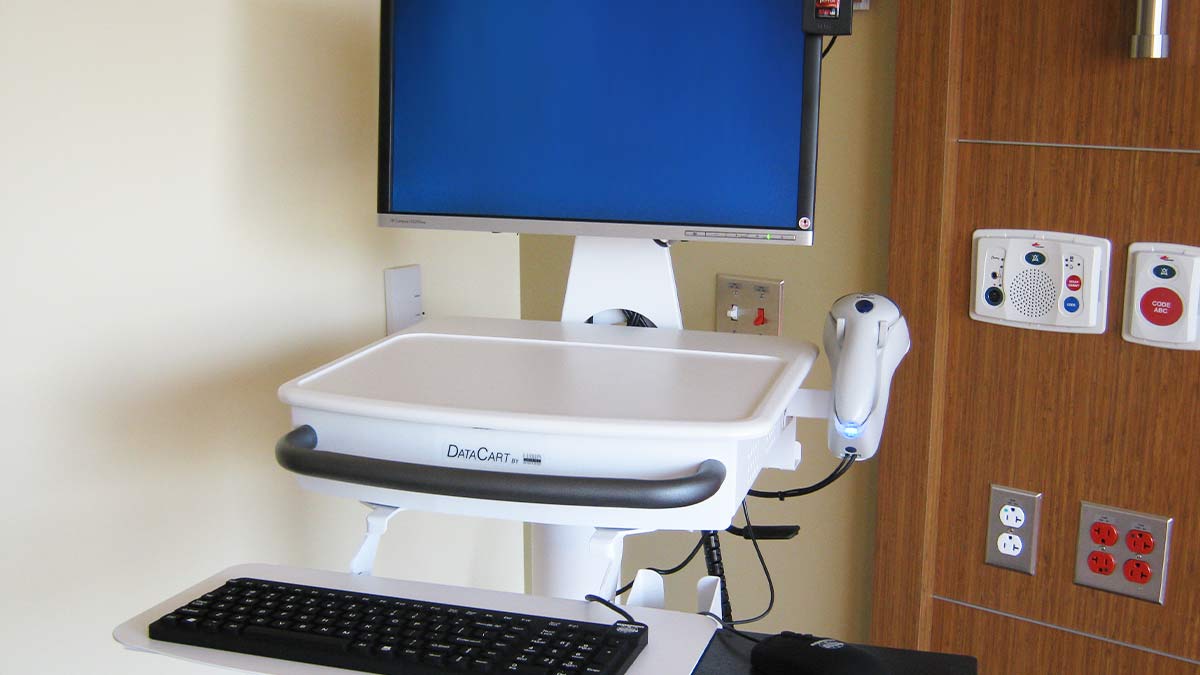
6.2) Electrical Safety and Charging Considerations
Checklist:
- Integrated power systems that meet UL 60601-1 or applicable standards
- No use of non-compliant extension cords or residential power strips
- Proper cord and plug integrity
Selecting carts with compliant, integrated power systems helps reduce electrical safety risks.
7) TJC Medical Equipment Requirements: Medication Delivery
Medication management standards are detailed and stringent. Below are general equipment-focused considerations.
7.1) Medication Storage and Security
Checklist:
- Locking medication carts and cabinets
- Separation of controlled substances
- Documented expiration date checks
Selecting carts with secure locking mechanisms and smooth cleanable surfaces simplifies compliance for pharmacy and nursing leadership.

8) TJC Medical Equipment Requirements: Electrical Safety and UL Standards
Electrical compliance is a frequent survey focus area, particularly in patient care spaces.
8.1) UL Listing and Certification
Checklist:
- Electrical and mechanical integrity verified and documented
- UL or equivalent certification confirmed
- Alignment with NFPA code requirements
Buyers should verify certifications prior to purchase, especially for power strips and integrated equipment assemblies.
8.2) Safe Use in Patient Care Areas
The following requirements apply within six feet of the patient bed, chair, or table.
Checklist:
- Power strips are used only on movable medical equipment and are permanently attached
- Compliance with UL 1363A or UL 60601-1 where applicable
- Not used for personal electronics
- Proper grounding and plug integrity
- Damaged cords removed from service
Electrical compliance is not just a facilities issue. It begins at the purchasing stage, especially when departments independently source power accessories or add components to existing assemblies.
9) What To Do After Receiving New Equipment
Accreditation risk does not begin at the time of a survey. It often begins the day equipment is delivered and placed into service.
Healthcare buyers, IT teams, and clinical engineering departments should have a standardized intake process for all newly received equipment.
9.1) Electrical Safety Testing
Before placing equipment into clinical use:
- Perform initial electrical safety testing per facility policy
- Verify grounding and plug integrity
- Confirm alignment with applicable UL and NFPA requirements
This step is especially important for devices that will be used within patient care areas or connected to other equipment assemblies.
9.2) Obtain and Retain Manufacturer Documentation
Every piece of equipment should be accompanied by:
- Manufacturer cleaning and disinfection instructions
- Preventive maintenance recommendations
- Technical specifications and certifications
Request, print, and retain these documents as part of your equipment file. Surveyors frequently ask how equipment is cleaned and maintained. Having manufacturer guidance readily available strengthens compliance.

9.3) Integrate Into Preventive Maintenance Programs
Before deployment:
- Add the device to your CMMS or tracking system
- Assign preventive maintenance frequency
- Identify whether the equipment qualifies as high-risk or life-support
Purchasing equipment without a clear path to maintenance integration can create documentation gaps later.
10) Staying Survey Ready
Accreditation readiness is a year-round process, not a pre-survey scramble.
Proactive steps include:
- Conduct mock inspections using official guidance from your accrediting agency
- Replace non-compliant equipment such as porous wood furniture proactively
- Standardize documentation across departments
- Confirm manufacturer cleaning and maintenance instructions at the time of purchase
Most importantly, partner with equipment providers who understand accreditation expectations and can help you select products that align with infection prevention, electrical safety, and documentation requirements.
11) Frequently Asked Questions
Asset tags are not explicitly required. What is required is the ability to identify equipment in your inventory and trace it to maintenance and inspection records. Many facilities use asset tags or barcode systems as a practical way to support identification, tracking, and documentation.
Survey focus is typically on whether surfaces are cleanable and non-porous. If a cart or furniture surface cannot be appropriately disinfected, or if it has deteriorated in a way that affects cleanability, it can create infection prevention concerns and potential findings. Facilities commonly replace porous or difficult-to-clean surfaces as a result of TJC walkthroughs.
In patient care areas, requirements are more restrictive. Power strips are generally expected to be used only on movable medical equipment and to be permanently attached, with appropriate UL standards depending on the application. Facilities should verify compliance with their Environment of Care and Facilities policies, and confirm manufacturer guidance and applicable UL standards before deployment.
Frequency is typically defined by facility policy and may vary by department and risk level. The key survey expectation is that cart checks are performed consistently, documented, and that the emergency cart remains readily accessible for immediate use.
Buying equipment that lacks clear maintenance documentation, is difficult to clean, or introduces electrical safety and accessibility concerns can force departments to create workarounds and purchase additional equipment. Over time, those workarounds increase compliance burden and create more points of failure during survey tracers.
Joint Commission Expertise at Convergint-Innovative Medical
If you are reviewing medical carts, OB equipment, medication storage, or electrical compliance across your facility, our team can help assess your current equipment and identify alternatives designed for healthcare environments.
Contact Convergint-Innovative Medical to schedule a call and reduce your survey risk before your next accreditation cycle.